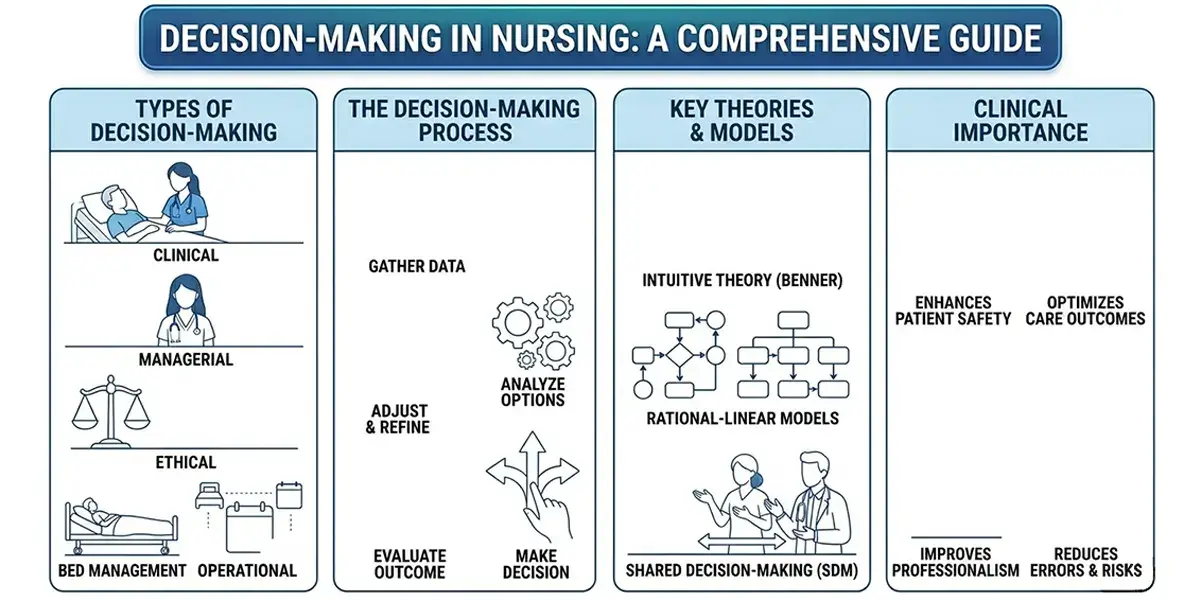
Healthcare requires quick decision-making, medical insight, and logical thought. Nurses are known to make very direct decisions that influence patient safety, treatment outcomes, and the efficiency of healthcare provision among healthcare professionals. In turn, decision-making in nursing is one of the essential professional competencies, which combines knowledge, clinical expertise, ethical responsibility, and evidence-based practice.
Healthcare organisations and hospitals operate in dynamic environments characterised by changing conditions. Nurses determine symptoms, analyse patients’ reactions, prioritize patient care, organize work with medical teams, and address emergencies. All the activities require an organized process of judgment based on professional training and clinical experience.
A well-developed decision-making process enables nurses to provide safe care to patients, improve the outcomes of their healthcare services, and work as a team member with other professionals. If you want to develop good decision-making skills, then you have to get an insight into the overall idea of decision-making and how it is applicable in nursing practice.
What Does Decision Mean? Understanding Decision Making
A decision is the choice of the best available alternative to achieve a given goal. In the work environment, decision-making involves examining available information, considering possible consequences, and choosing the most competent course of action.
The definition of decision-making in organizations describes it as a systematic thinking process used to address issues and guide behavior toward desired outcomes. Decision-making is essential in every professional field because people are constantly faced with situations that demand judgment, prioritisation, and problem-solving.
There are a number of critical aspects that are typically involved in decision-making:
- Identifying a problem or situation
- Gathering relevant information
- Evaluating possible solutions
- Selecting the most appropriate option
- Implementing the chosen action
- Reviewing results and outcomes
In a medical facility, the level of responsibility during decision-making is greatly heightened because the outcomes directly affect patient health and safety. Medical workers need to assess clinical data, analyze patient complaints, and select treatment based on scientific evidence.
Critical thinking, ethical awareness, the use of knowledge, and situational judgment are the attributes of effective decision-making in professional practice. In particular, nurses rely on these competencies because they are in constant contact with patients and actively involved in patient care.
What Is Decision-Making in Nursing?
Decision-making in nursing refers to the professional process by which nursing experts evaluate patients’ conditions, review treatment options, and determine the appropriate clinical measures to improve patient outcomes.
Decision-making and nursing cannot be separated because nurses are direct healthcare providers who constantly monitor patients’ health status. They observe symptoms, analyze clinical signs, manage contacts with doctors, and organize care plans; all of these operations require sound judgment.
- Clinical knowledge and professional training
- Evidence-based practice guidelines
- Patient assessment data
- Ethical principles
- Healthcare policies and protocols
In the case of a patient with the observed symptoms (when his condition is worsening), the nurse should check the vital signs, diagnose possible complications, and inform the appropriate medical unit. Moreover, the nurse must prioritize care actions by urgency.
This fact becomes even more obvious when the patients’ safety is considered. Nursing judgment is required in the administration of medications, the control of infections, the monitoring of patients, and emergency measures.
The development of strong decision-making skills remains an important aspect of nursing education and professional growth.
Importance of Clinical Decision-Making in Nursing
Clinical decision-making in nursing entails how nurses analyze patient data, synthesize clinical evidence, and select care interventions to improve patient outcomes.
Clinical settings require ongoing decision-making; nurses are expected to act quickly and promptly to support patients and prevent harm and mistakes.
Here are key areas where clinical decision-making is very crucial. They include:
Patient Assessment
The nurses assess patients’ conditions by observing, monitoring vital signs, and reviewing medical histories. The results of such an assessment can be used to inform treatment priorities and care planning.
Treatment Interventions
The treatment plans are developed by healthcare teams; however, nurses actively participate in implementing and modifying interventions. Nurses check patient reactions to drugs, treatments, and interventions.
Emergency Response
Clinical emergencies require swift action. Nurses observe warning signs of respiratory distress, abnormal vital signs, or changes in neurological status and take appropriate actions.
Care Coordination
Healthcare delivery involves multiple professionals, including doctors, therapists, pharmacists, and support staff. Nurses coordinate patient care and ensure communication between team members.
Patient Advocacy
Nurses advocate for patients when treatment plans require clarification or when patients need additional support. Advocacy decisions protect patient rights and well-being.
What are the 8 types of decision-making?
There are eight kinds of decision-making, including:
- Strategic decisions
- Tactical decisions
- Operational decisions
- Programmed decisions
- Non-programmed decisions
- Intuitive decisions
- Analytical decisions
- Collaborative decisions
Strategic Decision-Making
The focus of strategic decision-making is on the long-term goals and the general direction of the healthcare organizations. These are the decisions usually made by hospital administrators, top nursing executives, and health care executives. The decisions made by the healthcare institutions are influenced by strategic decisions.
They include the design of patient-safety programs, the implementation of new technologies in healthcare, staffing models, and the distribution of funding between departments. Irregular planning also requires careful consideration of healthcare trends, regulatory requirements, and organizational objectives.
Given their implications for the entire healthcare system, research, policy analysis, and leadership consultation usually support decisions.
Tactical Decision-Making
Tactical decision-making involves translating strategic plans into concrete actions within departments or units. These decisions are usually made by nurse supervisors, department managers, and clinical coordinators.
A nursing manager can, for example, schedule personnel, allocate resources in the wards, introduce new clinical guidelines, or reorganize the work process to increase efficiency.
Tactical decisions ensure that the organization’s strategic objectives are achieved at the departmental level. They need to be coordinated, led, and understand the day-to-day operational issues in a healthcare setting.
Operational Decision-Making
The operational decision-making process occurs in the daily care of patients and is the most common type of decision nurses make. These decisions focus on direct clinical actions and direct patient care activities.
They may include following a patient’s symptoms, delivering medication, prioritizing care processes, and responding to changes in a patient’s condition.
Nurses implement operational decisions based on clinical guidelines, patient evaluation, and professional judgment. These decisions may seem routine; however, they are extremely critical because they directly affect patient outcomes and safety.
Intuitive Decision-Making
Intuitive decision-making is a clinical experience and professional expertise. Skilled nurses develop the habit of identifying trends in patients’ conditions without necessarily examining every detail.
For example, a nurse can quickly identify the initial signs of patient decline based on minor symptoms or changes in behaviour.
Such intuitive knowledge enables medical workers to act quickly in emergency cases, and intuition is enhanced over time as nurses experience a range of clinical cases and develop trust in their professional judgment.
Analytical Decision-Making
Analytical decision-making is a systematic method that relies on facts, data, and logical appraisal. In this approach, nurses who adopt the strategy pay close attention to patient facts, laboratory data, and medical instructions before choosing the best course of action.
This is normally done by comparing the treatment options, evaluating the risk that it might bring, and following the evidenced based practice.
Analytical decision-making is particularly important when handling complex medical cases, which require careful evaluation to ensure accurate clinical judgment and effective management.
Programmed Decision-Making
Programmed decision-making is defined as repetitive decisions that follow defined procedures or protocols. Standardized policies are used in healthcare settings to regulate many clinical activities to ensure consistency and patient safety.
Some of them are infection-control measures, medication administration procedures, and admission procedures for patients. Since these processes are well-defined, health practitioners will be able to react quickly and with confidence, without having to develop a new solution for every case.
Non-Programmed Decision-Making
Non-programmed decision-making occurs when healthcare professionals face new or unexpected situations for which they do not have a set solution. It requires creativity, critical thinking, and judgment in such decisions.
As an example, it can entail handling uncommon medical issues, handling unusual complications of patients, or solving unexpected ethical concerns. In such cases, nurses must gather the relevant data, consult with colleagues, and evaluate potential outcomes before choosing the best strategy.
Collaborative Decision-Making
Collaborative decision-making involves teamwork and effective communication. Patient care is often a field of work that requires the contributions of nurses, physicians, pharmacists, therapists, and other experts.
With a team effort, the medical teams would share knowledge, discuss therapeutic options, and collectively determine the most suitable treatment option.
The approach will refine decision-making accuracy, reduce the risk of errors, and ensure that patients’ needs are met through various professional perspectives.
Decision-Making Theory in Nursing
Healthcare is a profession where professionals need to make decisions promptly, analyze correctly and make ethical decisions. The nursing practice requires making decisions based on clinical knowledge, assessment of the patient, evidence-based practice, and health care planning.
Rational Decision-Making Model
The structured decision-making process allows nurses to evaluate the situation of a patient, prioritize it, and arrange care in collaboration with care teams. The academic models and decision theories support clinical judgement, but the decisions supporting the management of the healthcare system are based on leadership decisions.
Intuitive Decision-Making Theory
Acquisition of good decision-making skills would assist nurses to deliver safe patient care, promote better healthcare and champion the healthcare systems.
Evidence-Based Decision Models
It requires evidence-based learning and reflection practice as well as continuous professional development to make sure that clinical decision-making is high among nursing professionals.
Evidence-based practice in nursing enhances the quality of clinical decisions by integrating scientific studies and clinical knowledge.
Reflective Decision Making
Reflective practice gives nurses the power to evaluate past clinical experiences and improve on decisions in the future. Professional reflection models also help evaluate actions and identify opportunities to learn. One common model is the Gibbs Reflective Cycle that allows professionals to go through the process of reflection, evaluation, and improvement.
Decision-Making Process in Nursing
Choosing in nursing is among the important professional spheres that directly influence patient outcomes, safety, and efficiency of health-care delivery. The nurses operate in the dynamic milieus, where they have to make decisions based on complex information, schedules and decisions made at the opportune time.
A structured decision-making process can help nurses to reduce errors and enhance patient satisfaction, as well as evidence-based care. This process can be researched using the significant aspects and steps of effective nursing decisions.
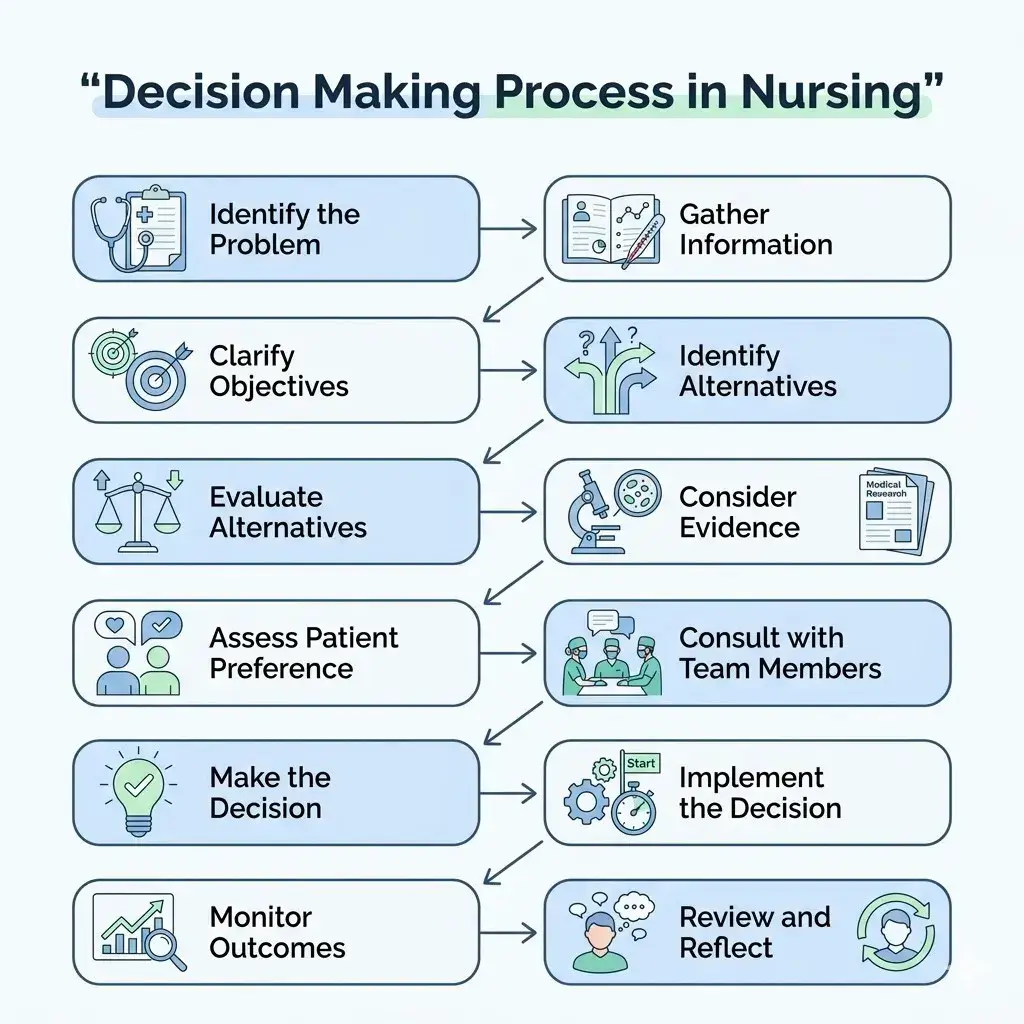
What are the 12 Steps in Decision-Making?
Here are the 12 steps in decision-making in nursing:
- Identify the Problem
- Gather Information
- Clarify Objectives
- Identify Alternatives
- Evaluate Alternatives
- Consider Evidence
- Assess Patient Preference
- Consult with Team Members
- Make the Decision
- Implement the Decision
- Monitor Outcomes
- Review and Reflect
Let’s have a look at them in detail.
Identify the Problem
The initial step in the nursing decision-making process is recognizing a problem and defining it properly. This entails close observation of the patient, the changes in conditions, or the absence of care. Identifying the problem makes sure that the next steps will be developed in accordance with the relevant problem and prevent working in another direction.
To illustrate, a nurse will be able to notice that a patient experiences uncontrolled pain and has to evaluate and treat it as soon as they can.
Gather Information
After having identified the problem, the nurses will be expected to collect deep and pertinent information. This would encompass reviewing the medical history of a patient, the recent lab, the history of medication as well as the vital analysis. The results attained during communication with a patient are required as well. The collection of precise data will give the nurses the full image of the situation and will make it possible to make decisions based on evidence rather than speculations.
Clarify Objectives
Nurses are expected to define the desired outcomes of the decision before finding solutions. The goals are supposed to be patient-related, specific, and measurable. They may include stabilisation of vital parameters, minimization of the risk of infection, or enhancement of overall comfort. Good goals are also clear and serve to guide and prioritize interventions.
Identify Alternatives
After establishing the goals, nurses are expected to enumerate all the potential actions. The potential options may be in the form of pharmacological treatments, non-pharmacological treatment, lifestyle adjustments, and specialized treatment. The communication of different options would guarantee the selected one to be informed and specific to the case of the patient.
Evaluate Alternatives
Each of the identified options should be studied in detail as to its possible benefits and drawbacks. The nurses need to take into consideration risks, feasibility, available resources, and anticipated outcomes.
This is exemplified by one treatment being effective and requires equipment unavailable; the other being a less urgent but safer treatment. The evaluation assists in selecting the most preferable alternative.
Consider Evidence
Modern nursing relies on evidence-based practice. The nurses will be required to consult clinical guidelines, research studies, and professional recommendations pertinent to the situation. This action is aimed at making sure that the decisions given are scientifically justified and are on the most current best practices, thereby minimizing the cases of errors and maximizing the amount of care provided to the patient.
Assess Patient Preference
The concept of patient-centred care assumes that the nurse should take into account patient values, beliefs, and personal preferences as well. These may either be cultural factors, past treatment experiences or willingness to participate in some interventions. The involvement of the patients makes the decision-making process more effective in terms of compliance, satisfaction, and overall results.
Consult with Team Members
Healthcare is a collaborative process. Nurses have an obligation to refer to physicians, specialists, other nurses, and other health assisting practitioners when necessary. Multidisciplinary consultation offers additional knowledge and insights to make sure the intervention adopted does not contradict the general care plans and organizational policies.
Make the Decision
A nurse makes a final decision after evaluating all the possibilities, analyzing the evidence, and consulting with the team on the matter. This is the decision which should be effective, safe and in accordance with the preferences of patients and available resources. It is important that the decision is recorded properly to be accountable and discuss it with the healthcare staff.
Implement the Decision
The action strategy adopted is put into action. Care should be planned, treatments provided, the patient and their family educated and adherence to the established protocols must be followed. At this point, nurses are expected to be adaptable and to be willing to change interventions in case of any unforeseen complications.
Monitor Outcomes
The nurses are regularly evaluating whether the patient is responding to the decision that has been implemented. Observation refers to the process of studying the vital signs, laboratory results, and modification in symptoms and the general well-being of the patient. The prompt assessment will also help to realise the positive outcomes and the intervention will be corrected in case it is not effective.
Review and Reflect
The last one is an evaluation of the decision making process. Nurses will be expected to reflect on what worked, what did not work and how the result might have been better. The reflections create professional development, the decisions of the future, and the improvement of patient care even more.
These steps will help to approach the clinical decision-making process comprehensively and minimize errors and provide high-quality care.
Decision-Making in Nursing Leadership
The healthcare systems are based on the presence of effective leadership in maintaining the safety standards, improving patient outcomes, and managing healthcare resources. Nursing leadership decision-making focuses on administrative and managerial roles.
Nurse leaders engage in strategic decision-making related to the management and coordination of staff in healthcare settings.
- Staffing Decisions: The allocation of staff by hospital administrators and nurse managers depends on patient needs, ward capacity, and the distribution of work.
- Patient Safety Policies: Nurse leaders make policies that reduce the risks in clinical settings, enhance the process of infection control, and enhance the quality of healthcare.
- Healthcare Resource Management: Medical institutions have limited resources; nurse leaders manage both equipment distribution and medication supplies, as well as budgetary limitations.
- Conflict Resolution: Professional teams in healthcare include professionals from different fields. Nurse leaders address workplace conflicts and guarantee collaborative care provision.
Leaders’ decisions affect organizational healthcare outcomes. Effective nurse leaders can apply clinical skills and managerial competencies to lead healthcare teams.
Decision-Making in Nursing Examples
You can see the importance of decision-making in nursing through the real-world scenarios.
Prioritizing Patient Care:
A nurse with several patients has to give care activities based on urgency as a priority. A patient with breathing difficulties must be treated urgently rather than undergo regular monitoring.
Medication Administration
Nurses assess patients’ allergies, drug interactions, and the correctness of dosage before administering medications. Healthcare teams are required to communicate, and this is a responsibility of the nurse to maintain consistent dialogues with them.
Communication with Healthcare Teams
Nurses report the change of patient condition to physicians, pharmacists, and therapists. Effective communication facilitates proper treatment decisions.
Patient Education
Nurses give patients guidelines related to using drugs, rehabilitation, and lifestyle changes.
The above decision-making in nursing examples demonstrate the practicality of the application of clinical judgment in the healthcare setting.
FAQs
What is decision-making in nursing?
Decision-making in nursing refers to the professional process nurses use to assess patient conditions, evaluate treatment options, and select appropriate care interventions.
What are the three main types of decision-making?
The three primary types include strategic decisions, tactical decisions, and operational decisions.
What are the 8 types of decision-making?
Strategic, tactical, operational, programmed, non-programmed, intuitive, analytical, and collaborative decisions.
What does decision mean?
A decision represents the selection of one option among several alternatives in order to solve a problem or achieve a goal.
What are the 7 elements of decision-making?
Problem identification, information gathering, generating alternatives, evaluating options, selecting solutions, implementation, and evaluation.
What are the 12 steps in decision-making?
The twelve steps include identifying the problem, collecting data, analysing options, selecting solutions, implementing interventions, and evaluating outcomes.
Why is clinical decision making important in nursing?
Clinical decision making ensures patient safety, improves treatment outcomes, and supports effective healthcare teamwork.
What are decision-making theories in nursing?
Common theories include rational decision models, intuitive decision frameworks, and evidence-based decision models.
How do nurses improve decision-making skills?
Continuous education, clinical experience, evidence-based practice, and reflective learning improve nursing judgement.
What role does leadership play in nursing decisions?
Nurse leaders guide policy implementation, manage healthcare teams, and ensure patient safety across healthcare organizations.
Final Thoughts
Healthcare is a profession where professionals need to make decisions promptly, analyze correctly and make ethical decisions. The nursing practice requires making decisions based on clinical knowledge, assessment of the patient, evidence-based practice, and health care planning. The structured decision-making process allows nurses to evaluate the situation of a patient, prioritize it, and arrange care in collaboration with care teams.
The academic models and decision theories support clinical judgement, but the decisions supporting the management of the healthcare system are based on leadership decisions. Acquisition of good decision-making skills would assist nurses to deliver safe patient care, promote better healthcare and champion the healthcare systems.
It requires evidence-based learning and reflection practice as well as continuous professional development to make sure that clinical decision-making is high among nursing professionals.